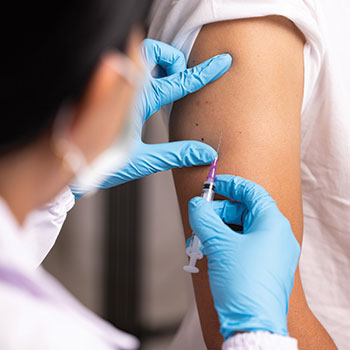
Combating the crisis of loneliness
While the COVID-19 pandemic put a spotlight on loneliness, social engagement with friends and family has been falling for the past two decades as feelings of social isolation have increased.
There's a newly declared epidemic that is harming health and contributing to mortality—loneliness and a lack of social connection—and primary care physicians are on the front lines.
U.S. Surgeon General Vivek H. Murthy, MD, recently declared loneliness an epidemic with a mortality impact equivalent to smoking up to 15 cigarettes a day. While the COVID-19 pandemic put a spotlight on loneliness, social engagement with friends and family has been falling for the past two decades as feelings of social isolation have increased, according to the Surgeon General's Advisory.

The Advisory, which was released in May 2023, outlines the consequences of inadequate social connection, which include not only an increased risk for depression and anxiety but significant increases in the risk of premature death, stroke, and heart disease, among others.
“It's all the major things that we as internists see in practice,” said Carla Perissinotto, MD, MHS, a geriatrician and professor of medicine at the University of California, San Francisco, whose own research has shown that among older adults, loneliness was a predictor of both functional decline and premature death.
Dr. Perissinotto said it's critical that internal medicine physicians get involved in routinely assessing loneliness and addressing it. “As a primary care clinician, I am very aware of the number of things we are asked to do. I would argue that there are many things we're asked to do that may not be as meaningful to patients directly as loneliness,” she said.
A national strategy
The Surgeon General's Advisory proposes a National Strategy to Advance Social Connection that includes investments in parks, playgrounds, and community programs, as well as national policies such as expanded public transportation and paid family leave. Reexamining the role of technology and funding research into the causes and consequences of social disconnection are also on the Surgeon General's agenda.
The health care sector plays a key role in the national strategy. The Advisory recommends educating clinicians on the physical and mental health benefits of social connection and the health risks associated with loneliness. It also calls for assessing social isolation and loneliness in patients and providing support by linking patients with community-based organizations.
The Surgeon General isn't the only one highlighting the issue of loneliness. In early 2020, the National Academies released a consensus study report that explored the evidence base around social isolation and loneliness in adults ages 50 years and older and recommended using validated tools to periodically assess at-risk individuals. Globally, both the United Kingdom and Japan have appointed ministers of loneliness to help lead their national efforts to combat social isolation. The World Health Organization is also working on interventions to address social isolation and loneliness in older adults.
Who is at risk?
While loneliness can affect anyone at any age, research suggests that some groups are at higher risk, such as individuals with poor physical or mental health, those with disabilities, individuals experiencing financial insecurity, individuals who live alone, and both older and younger adults, the Surgeon General's Advisory said. Other groups with increased risk may include individuals experiencing discrimination, such as those in ethnic and racial minority groups and LGBTQ+ individuals, according to the Surgeon General's Advisory.
Traditionally, older adults were considered at highest risk for loneliness, but research over the last five years suggests that it may actually be younger adults, Dr. Perissinotto said. She noted, however, that older adults are at greater risk of experiencing the consequences of loneliness, which can compound the increased risk of cognitive impairment, heart disease, and other conditions that are more common in older age. “It's actually the entire lifespan we need to look at,” she said. “A simple way of thinking about it is that losses predict loneliness.”
Those losses could include the loss of a partner through death or divorce, the loss of a job, the loss of community following a move, or loss of mobility or function, such as hearing impairment, she said.
Women can be vulnerable to loneliness at several points in their lives, including childbirth, said Eileen West, MD, FACP, an internal medicine physician who specializes in women's health in Fairfax, Va. “Having a baby can be a very isolating experience because you spend all day meeting the needs of your child. Even with your spouse or your closest contacts, suddenly the conversation is all about the baby,” she said. “Women experience loneliness a lot after childbirth.”
The years of physical changes that accompany menopause and the period when children leave the house, which can cause a shift in family dynamics and social networks, are also times when women are at risk for episodes of loneliness, Dr. West said.
Assessing social connection
When it comes to assessing patients for loneliness, Dr. Perissinotto recommends screening annually and following major life events. There are validated tools for measuring loneliness and social isolation, including the UCLA 3-Item Loneliness Scale, the 6-item de Jong Gierveld (dJG) Loneliness Scale, and others.
Dr. Perissinotto favors the UCLA-3, which asks patients to rate their feelings of isolation, feeling left out, and lacking companionship. She said the questionnaire is brief and easy to use, and she includes the results in the patient's electronic health record.
Maria Torroella Carney, MD, FACP, chief of the division of geriatrics and palliative medicine at Northwell Health in New Hyde Park, N.Y., said she can often get a sense of a person's support network and their feelings of loneliness when reviewing their independent activities of daily living. She also starts her patient visits by asking: “If I could help you with one thing, what would it be?”
“That open-ended question often surprises me because the answer could be, ‘I'm lonely,’ or ‘I'm sad,’ or ‘Help me get out of my house,’” Dr. Carney said.
No ‘one-size-fits-all’ prescription
There's no easy prescription to combat loneliness, and providing concrete recommendations for patients experiencing loneliness is a challenge, experts said.
“A lot of health care providers are reluctant to have the conversation, in part because of the stigma, in part because they don't know what to do with the answers,” said Evan M. Benjamin, MD, MS, FACP, associate professor of medicine at Harvard Medical School and associate professor of health policy and management at Harvard School of Public Health in Boston. “It's the same thing we see around social determinants of health: We know it has an impact on health, but if we don't have a good screening and a good referral, it makes providers reluctant.”
Dr. Benjamin has been involved in formulating strategies to mitigate the impact of loneliness in New York City as part of a project between the city and Ariadne Labs, a health care innovation center at the Harvard School of Public Health and Brigham and Women's Hospital. One of the early lessons from the project was the need to normalize loneliness so that patients would be more comfortable discussing it and asking for help.
“Start with you, your office, and your staff. Every interaction with a patient is a moment to connect,” he said. “Providers are uniquely suited to recognize loneliness and they should be comfortable talking about it and normalizing it so we can then seek intervention.”
Dr. Perissinotto recommended using the framework from the Surgeon General's Advisory to help tease out where patients need support.
The Advisory breaks down the elements of social connection into three components:
- structure, or the number and variety of relationships, such as household size and size of a patient's friend circle;
- function, or the degree to which a person can rely on others for their needs, such as support in a crisis or mentorship; and
- quality, or the quality of relationships and interactions, such as marital satisfaction or social inclusion.
“That structure is really helpful for clinicians to think about addressing this,” Dr. Perissinotto said. For example, if the number of social connections is an issue, the patient may benefit from going to a senior center or joining a community organization. However, if the quality of a marital relationship is poor, couples' counseling might be a better answer, she said.
“It's very much like other things in medicine where there's a menu of options and it's about trying to think through what's driving the loneliness. Where we have failed before is the one-size-fits-all approach,” Dr. Perissinotto said.
Dr. Carney starts by asking about family relationships and then works with social workers in her health system to find out what resources are available to the individual patient, such as veterans' programs or adult day programs. For patients older than age 60 years, the Eldercare Locator, a public service of the U.S. Administration on Aging, can provide information on programs by ZIP code. For patients who are still working, there may be additional resources through their employers, she said.
“For many internists, it's very hard to understand what's available to that patient in their ZIP code. We have to do a better job to help clinicians link to these resources to help their patients,” Dr. Carney said.
Technology may also provide some help for seniors experiencing loneliness. A pilot project between the New York State Office for the Aging and Intuition Robotics has been using a robotic companion, powered by artificial intelligence, to initiate conversations and suggest activities with older New Yorkers. Over the last year, use of the AI companion was associated with a 95% reduction in loneliness. “There's this innovative world of technology that we might be able to offer in the near future,” Dr. Carney said.
Dr. West said a loneliness prescription can also be small and personal. For instance, when seeing a patient who was experiencing loneliness after the loss of a spouse, she asked the woman if she'd like to be the family member who always remembers everyone's birthdays. “A lot of times happiness and sadness can be influenced by taking the focus off yourself and realizing that you might actually be better off than someone else,” Dr. West said.
Some patients may be resistant to addressing their feelings of loneliness. In that case, clinicians can provide education and return to the topic later, similar to the approach used with smoking cessation, Dr. Perissinotto said. “What we need to get comfortable saying is that we don't have to solve all things in one day, and it's a stepwise approach,” she said.