MKSAP Quiz: 3-year history of erythema, flaking
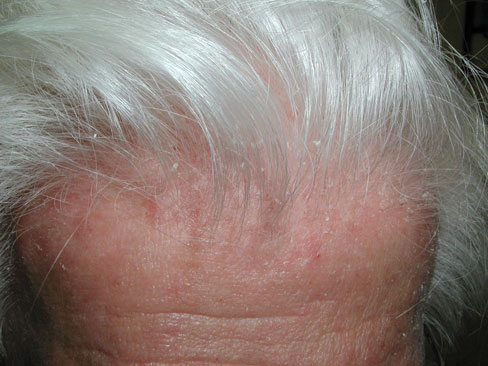
A 78-year-old man is evaluated for a 3-year history of erythema and flaking on the scalp and face.
On physical examination, ill-defined greasy, yellow to erythematous patches with slight scale are noted on the eyebrows, nose, and medial aspects of the cheeks. Similar changes on the scalp are shown. There are no additional skin or nail changes.
Which of the following is the most appropriate treatment?
A. Clindamycin lotion
B. Clobetasol ointment
C. 5-Fluorouracil cream
D. Oral ketoconazole
E. Zinc pyrithione shampoo
Answer and critique
The correct answer is E. Zinc pyrithione shampoo. This content is available to MKSAP 19 subscribers as Question 12 in the General Internal Medicine 2 section.
The most appropriate treatment is zinc pyrithione shampoo (Option E). This patient has a classic presentation of seborrheic dermatitis, a common condition characterized by greasy, scaly, yellow to erythematous patches in seborrheic areas (scalp, face, ears, upper chest, axillae, and inguinal folds). On the face, specific areas of involvement include the eyebrows, medial aspects of the cheeks, inter-eyebrow region, and nasal ala. Topical antifungal treatments are first-line treatment. Over-the-counter medications, such as zinc pyrithione and selenium sulfide shampoos, are the most cost-effective treatment options to use first. Ketoconazole shampoo and cream are also effective. Patients should apply the shampoo on the skin and allow it to sit for 5 minutes before rinsing it off. Seborrheic dermatitis is believed to be caused by heightened sensitivity to yeasts, such as Malassezia. It is more common in patients with neurologic disorders, such as Parkinson disease and Alzheimer dementia. Low-potency topical glucocorticoids can be used in combination with antifungal treatments when severe inflammation is present. Often, a low-potency topical glucocorticoid is added for flares.
Clindamycin lotion (Option A) is often used to treat acne and folliculitis, which are characterized by inflammatory papules and pustules; these are not present in this patient. Clindamycin is not effective for seborrheic dermatitis.
Clobetasol ointment (Option B) is an ultra-high-potency topical glucocorticoid and would not be appropriate treatment for this patient's seborrheic dermatitis. Furthermore, use of ultra-high-potency topical glucocorticoids increases the risk for skin atrophy and should not be used on the face. A low-potency topical glucocorticoid, such as hydrocortisone or desonide, can be used in combination with topical antifungal agents for treatment of seborrheic dermatitis flares.
5-Fluorouracil cream (Option C) is used to treat actinic keratosis and is not appropriate treatment for this patient. 5-Fluorouracil cream often exacerbates seborrheic dermatitis.
Oral ketoconazole (Option D) is not an appropriate treatment for seborrheic dermatitis or any superficial fungal infection. In 2016, the FDA issued a boxed warning for ketoconazole due to risk of liver and adrenal toxicity and interactions with other medications. The use of systemic ketoconazole is limited to the treatment of susceptible systemic fungal infections (blastomycosis, histoplasmosis, paracoccidioidomycosis, coccidioidomycosis, and chromomycosis) in patients in whom other, safer antifungal therapies have failed or who are intolerant to such therapies. Rarely, in refractory cases of seborrheic dermatitis, oral antifungals can be considered; in these cases, fluconazole would be preferred because of the lower risk for side effects.
Key Points
- Cost-effective treatment of seborrheic dermatitis, a common condition characterized by greasy, yellow, scaly, yellow to erythematous patches in seborrheic areas, includes zinc pyrithione or selenium sulfide shampoos.
- Oral ketoconazole is not an appropriate treatment for any superficial fungal infection.




