MKSAP Quiz: 1-month history of rash
A 52-year-old woman is evaluated for a 1-month history of a spreading rash on her back, chest, and arms. She has been using over-the-counter topical glucocorticoids without relief. She does not have any other associated symptoms and otherwise feels well. Medical history is significant for hypertension. Medications are hydrochlorothiazide and metoprolol.
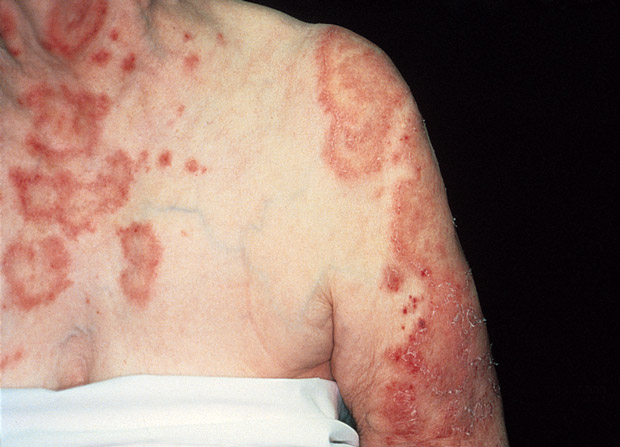
On physical examination, temperature is 37.1°C (98.7°F), blood pressure is 141/83 mm Hg, pulse rate is 72/min, and respiration rate is 18/min. Skin findings are shown.
There are no lesions in the scalp or ears, no finger or nail changes, no joint inflammation, and no oral ulcers. The remainder of the physical examination is unremarkable.
Laboratory studies:
| Antinuclear antibodies | Positive (titer of 1:320) |
| Anti-Ro/SSA antibodies | Positive |
| Anti-La/SSB antibodies | Negative |
| Antihistone antibodies | Negative |
| Creatine kinase | Normal |
Which of the following is the most likely diagnosis?
A. Dermatomyositis
B. Pemphigus foliaceus
C. Psoriasis
D. Subacute cutaneous lupus erythematosus
Answer and critique
The most likely diagnosis is D. Subacute cutaneous lupus erythematosus. This question can be found in MKSAP 17 in the Dermatology section, item 26.
This patient has a typical eruption of subacute cutaneous lupus erythematosus (SCLE). Although associated with systemic lupus erythematosus (SLE), it is a distinct disorder that may present with different cutaneous findings than those usually associated with SLE. There are two presentations of SCLE: annular scaly patches on the upper back and sun-exposed areas or a more psoriasiform eruption that can have less distinctive morphology but also occurs in sun-exposed areas. SCLE is associated with a number of medications believed to trigger the disorder, including hydrochlorothiazide, calcium channel blockers, ACE inhibitors, terbinafine, and the tumor necrosis factor α (TNF-α) inhibitors. This patient is taking hydrochlorothiazide, which was the first drug reported in association with SCLE and remains a common cause of drug-induced SCLE. Patients with SCLE tend to be very photosensitive, may have antinuclear antibody positivity, and are often positive for anti-Ro/SSA antibodies (and may be positive for anti-La/SSB antibodies). Patients with drug-induced SCLE may be antihistone antibody positive (about one third to one half of patients), but antihistone antibody positivity is not necessary to make the diagnosis. Compared patients with SLE, those with SCLE tend to have fewer systemic findings, although a subset of patients may have kidney involvement. Notably, all women with anti-ro/SSA and anti-La/SSB antibodies are at risk for having newborns with neonatal lupus, and pregnant patients or mothers of newborns with this pattern of skin eruption or serologic antibody profiles should be counseled and their babies screened accordingly. For drug-induced SCLE, discontinuing the inciting medication is essential to treatment.
Dermatomyositis may present without muscle inflammation, but this patient's skin eruption is characteristic of SCLE. The rash of dermatomyositis is accentuated around the eyes (heliotrope rash), around the lateral shoulders (“shawl sign”), and involves the knuckles of the metacarpal and interphalangeal joints (Gottron sign).
Pemphigus foliaceus is an autoimmune blistering disease in which the autoantigen is in the upper regions of the epidermis, leading to superficial blisters that rapidly rupture and cause dried crusts over inflamed skin, which have been described as looking like “cornflakes.” The morphology and distribution of the eruption described in this patient would be atypical, and patients with pemphigus foliaceus are not often positive for anti-Ro/SSA antibodies or high-titer antinuclear antibodies.
Psoriasis generally occurs over joints or at areas of trauma or friction, is not generally annular, and should not be photodistributed. Classic plaque psoriasis is characterized by pink plaques with silvery scale over the knees, elbows, and often around the umbilicus and gluteal cleft.
Key Point
- Patients with subacute cutaneous lupus erythematosus have annular scaly patches that are typically drug or sunlight induced.




