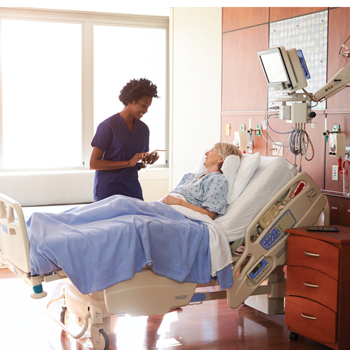
Abdominal wall pain as its own diagnosis
Internists can diagnose chronic abdominal wall pain with a simple physical exam and some savvy history taking, experts said, and reassure patients that their condition is not serious and may respond to treatment.
When investigating the source of abdominal pain, physicians might check the front and back doors but overlook the wall.
Of course, they recognize the signature pain patterns of classic diagnoses like pancreatitis and appendicitis, but not all abdominal pain comes from the viscera. If a patient's abdominal pain doesn't fit into a familiar paradigm, experts said it's worth considering the abdominal wall as a potential culprit.
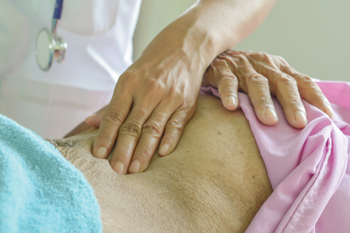
Patients with chronic abdominal wall pain (CAWP) are rarer than those with functional gut disorders like irritable bowel syndrome (IBS), and the underlying pathologies are quite disparate. Unlike IBS, CAWP does not cause gastrointestinal symptoms or altered bowel habits, though the two share abdominal pain as a common symptom.
Physicians, however, sometimes overlook CAWP as a possibility and instead give patients with abdominal pain symptoms (but normal diagnostic test results) another diagnosis, such as IBS or functional abdominal pain, said gastroenterologist Adam C. Ehrlich, MD, MPH, an assistant professor of medicine at Lewis Katz School of Medicine at Temple University in Philadelphia.
“This is one of those things that is very frustrating for both physicians and patients because you can do all the testing that you want, and you really don't find anything,” he said.
Oftentimes, finding nothing isn't for lack of trying. At Mayo Clinic in Rochester, Minn., gastroenterologist Madhusudan Grover, MBBS, has seen many cases of patients whose CAWP is unresolved despite visits to multiple physicians and subspecialists.
“It's one of the key diagnoses we look for in longstanding chronic abdominal pain. … Almost invariably, these are patients who have had symptoms for months to years, have undergone a number of tests for diagnosing what's causing the pain, and have been labeled as IBS and other entities,” he said.
Fortunately, just like the classic diagnoses, CAWP has a very specific presentation. Internists can diagnose CAWP with a simple physical exam and some savvy history taking, experts said, and reassure patients that their condition is not serious and may respond to treatment.
Pathophysiology
Understanding CAWP requires understanding the different functions of two types of nociceptors, the A-delta and the C, explained gastroenterologist George W. Meyer, MD, MACP, a clinical professor of internal medicine at the University of California, Davis. A-delta nerve fibers allow us to localize sharp pain with one finger, he said, whereas C fibers are involved in signaling the dull, vague pain of intra-abdominal symptoms.
This is a key difference between CAWP and functional gut disorders. Dr. Meyer said most patients with CAWP can point to the pain location with a single finger. In contrast, patients with intra-abdominal pain may localize the pain with one hand or by rubbing a large portion of his or her abdomen, he said.
In CAWP, the most common pain location is, by far, along the rectus sheath in patients with non-operated abdomens (anywhere along the lateral borders of the rectus abdominis muscles), said Dr. Meyer. Patients who have had operations on their abdomens also present with this pain syndrome but instead tend to report pain in the corner of a scar or at the insertion point of a laparoscopic procedure, he said.
Another historical feature that is classic for CAWP is that patients must constantly change positions to make themselves comfortable, said Dr. Grover. “It has a strong positional component,” he said. “Typically, they will tell you that when they lie down, things get much better.”
Dr. Meyer agreed that changing positions can often relieve patients' pain. “Many patients who sit at a desk or computer for a long time will notice the pain and can relieve it by standing up, walking around, or lying down,” he said. “The pain is often better during the weekend.”
To examine the abdominal wall, Dr. Meyer recommends first asking the patient to point with one finger to where it hurts the most. (A Stanford Medicine video explainer can be found online.) Then, using one finger, the physician applies pressure to the painful spot and asks the patient either to sit up or to raise both legs above the table at the same time, he said. The person with abdominal wall pain will experience an increase in pain, whereas patients with internal dysfunction may experience a decrease in their pain symptoms with muscular contraction.
This physical exam finding, which is classic for CAWP, is called Carnett's sign and is named after the surgeon who first described it in the 1920s, said Dr. Ehrlich. “It's been shown to be sensitive and specific to identifying this disorder and might prevent you from doing another colonoscopy or doing another CT scan or doing some other testing that may not be necessary,” he said.
Many physicians may not be familiar with Carnett's sign, said Dr. Meyer. “What's amazing is that people have been recognizing this [condition] for quite a while, and we don't teach the exam of the abdominal wall,” he said.
Although Dr. Ehrlich learned more about abdominal wall pain during his gastroenterology fellowship, he said new physicians still seem uninformed. “We have residents who are rotating through our services or our clinic, and they don't seem to be aware of that particular physical exam finding,” he said.
Carnett's test can help distinguish CAWP from pain of visceral origin, but Dr. Grover noted that he does not always require that patients demonstrate a positive Carnett's sign when deciding to treat with injection (more on that in a moment). This is because, in a retrospective study published in 2016 in Digestive Diseases and Sciences, he and his group found that Carnett's sign wasn't predictive of who may or may not get better with injection.
“I think it's a good idea to do Carnett's [test], but I don't think we should rule out the possibility of injecting them on the basis of Carnett's,” said Dr. Grover, also an assistant professor of medicine, physiology, and biomedical engineering at Mayo. If such components as localized pain, positional worsening, and nonassociation with meals are present, even with an equivocal or negative Carnett's test, he said he is typically inclined to recommend injection.
Dr. Meyer said that, in his experience, he can tell if an injection is going to work before the patient leaves the room. “Usually, I inject, finish my record on the computer, then return to the patient and, if the diagnosis is correct, the patient is pain-free,” he said.
Treatment
These days, the road to pain relief can be swift for patients with CAWP, although doctors have spent decades arriving at the correct formula.
In the mid-1970s, shortly after William V. Applegate, MD, a family physician, described anterior cutaneous nerve entrapment syndrome as one of the most frequent causes of CAWP, Dr. Meyer said he began to consider the diagnosis in his own patients with otherwise unexplained abdominal pain.
In an attempt to treat these patients, he injected them with lidocaine in the particularly tender areas along their rectus sheath. Patients got great relief, albeit temporarily. “I quit doing it in 1976 because after two hours, the pain would come back and become more severe,” said Dr. Meyer.
After reading a seminal 2002 article on CAWP management by Radhika Srinivasan, MD, FACP, and David S. Greenbaum, MD, FACP, in the American Journal of Gastroenterology, Dr. Meyer began injecting patients with triamcinolone in addition to lidocaine, after practicing for a decade or two without trying to intervene at all. “I had one woman call me ‘Dr. Merlin’ because she'd had this pain for 20 years and I was the first person to be able to relieve her pain,” he said.
In similar fashion, physical medicine and rehabilitation clinicians at Mayo perform ultrasound-guided injection of triamcinolone and bupivacaine, a long-acting anesthetic, to treat patients with CAWP, said Dr. Grover. Ultrasound guidance helps avoid futile injections (i.e., into the peritoneal cavity) and keeps the risk of complications low, he said, but no comparative trials have shown its efficacy versus nonguided injection.
A physician can safely learn to perform the injections, said Dr. Grover. “I've known of physicians who have used ultrasounds in their offices, as well, so it can be done if they feel comfortable from a safety aspect … I think injection, in the broad scheme of things, is much less harmful, invasive, and much more cost-effective than some of these other things we do,” he said.
But since many internists are not familiar with this type of treatment, known as trigger-point injections, Dr. Grover recommends referring patients to either a gastroenterologist or pain specialist if CAWP is suspected. “Gastroenterologists would be more familiar with the condition—at least, they would understand more promptly—but I think either can do a good job at it,” he said.
After all their unexplained pain, patients are usually willing to try injections, said Dr. Grover. “I have referred hundreds of patients, and I have not seen anybody being hesitant to it,” he said. “They think of it very similarly to a back pain injection or a knee injection. They actually feel quite relieved that it is something that's safe, can be done easily, and has the possibility of helping with the pain.”
After the procedure, which lasts about 20 to 30 minutes, pain relief varies from person to person but typically kicks in within 72 hours and lasts 12 to 16 weeks, Dr. Grover said. “If somebody has had a really wonderful response to the first injection and they then start losing that response, we have occasionally brought them back for a second and rarely for a third injection … but we typically don't repeat injections if [patients] haven't had a good response to the first one,” he said. If a week passes without improvement in the pain, then CAWP is probably the wrong diagnosis, said Dr. Grover.
It's also important to consider lifestyle triggers that compress the abdomen, he noted. If trauma was a precipitating factor, he said, one or two injections can usually get the job done. “But if it's a bus driver who's always going to be sitting in that position, I try to at least guide them toward some sort of work hygiene and positional hygiene,” such as stretching to relieve persistent pressure in the area, Dr. Grover said.
There is a dearth of evidence from randomized, controlled trials on the effectiveness of injecting the abdominal wall with lidocaine or a corticosteroid, Dr. Ehrlich noted. “There's some thought that just sticking a needle in might be helpful, without doing anything, because if there's fibrous tissue or scar tissue there, then the needle may break up the tissue and make things better,” he said. “But because there's no gold-standard diagnosis, part of the diagnosis is often response to injection.”
Although injection of lidocaine and triamcinolone is the generally accepted treatment, other options are available, said Dr. Ehrlich. Stretching, using a heating pad, taking nonopioid pain medication, and physical therapy can all be helpful in relieving CAWP, he said.
Dr. Ehrlich added that he is unaware of any long-term sequelae of untreated CAWP, so reassurance is key. “A lot of patients, their main worry (at least in my experience in the GI world) is that they have some cancer inside that is killing them slowly,” he said. “I start by telling people that this is not a serious condition … and just giving them that information is often a big help.”