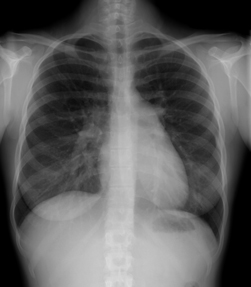
Don't overlook pulmonary hypertension
Learn how doctors can best spot pulmonary hypertension, a disease for which treatments have improved dramatically but inclusion in the typical internist's differential hasn't.
Treatment for pulmonary hypertension has improved dramatically over the past two decades, with nine FDA-approved therapies available where once there were none. But although early therapy is crucial to improved outcomes, the time between symptom onset and diagnosis still hovers at around two years, according to experts. Like other diseases that are a challenge to diagnose in primary care, pulmonary hypertension often mimics other, more common conditions, such as asthma. In addition, patients may chalk their symptoms up to lack of fitness and may not present to their physicians until late in the disease course. Read our story to learn more about when to suspect pulmonary hypertension and how to confirm the diagnosis.
Another story tackles an age-old question: How often do doctors follow the lifestyle recommendations they give their patients? Counseling on diet and exercise is commonplace in primary care, yet the time constraints of physicians' demanding jobs often make it difficult for them to practice what they preach. There's more than one reason to make an effort to do so, though, as good lifestyle choices not only improve physicians' own health but may also end up improving the care they provide their patients.
The recent devastation caused by Hurricane Sandy may have raised questions for physicians about what happens when their practices need to close unexpectedly due to a natural disaster. How should patients be informed? Where should they go for emergency care? How should appointments be rescheduled? And should office staff be paid regardless of the closure? Our story offers tips on how to keep things running as smoothly as possible during and after such a crisis.
Other features in this issue include stories on probiotics, vision loss in diabetics, and a program to improve primary care for sickle cell anemia, as well as an article about how EHRs can get in the way of efficiently stopping a patient's medication.
Finally, ACP will hold its annual meeting, Internal Medicine 2013, later this month in San Francisco. As always, the ACP Internist staff will be on site to bring you the latest news via our blog and our Twitter feed, as well as our daily e-mail dispatches. We'd love to meet you in person, so if you'll be in San Francisco, please stop by our booth at the ACP Resource Center. And as always, we're reachable any time by e-mail.
Sincerely,
Jennifer Kearney-Strouse