MKSAP Quiz: Cardioversion to restore normal sinus rhythm?
A 71-year-old man presents for a routine visit. He has a history of hypertension and atrial fibrillation. The atrial fibrillation was diagnosed 4 years ago when he had a transient ischemic attack. He reports feeling well and being able to do all his normal activities without limitation. He is an avid golfer. His current medications include metoprolol 100 mg/day, hydrochlorothiazide 25 mg/day, and warfarin adjusted to an INR of between 2 and 3.
His physical examination demonstrates a heart rate of 68/min and blood pressure of 122/78 mm Hg. The cardiac examination reveals an irregular rate with no murmur. There is no jugular venous distention or edema, and the lungs are clear to auscultation. The electrocardiogram is shown in the figure.
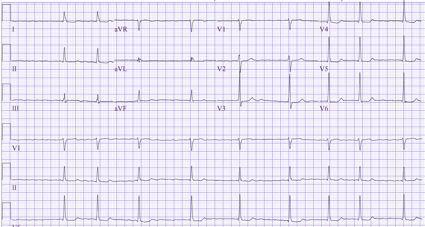
The patient has a friend who underwent cardioversion for restoration of normal sinus rhythm, and he wants to know whether restoration of sinus rhythm would be beneficial to him.
Which is the best management option for this patient?
A. Initiate amiodarone
B. Refer for pulmonary vein ablation
C. Schedule external cardioversion
D. Continue existing treatment
Answer and Critique
This item is available to MKSAP subscribers in Cardiovascular Medicine: Item 31.
In patients who tolerate atrial fibrillation well or are minimally symptomatic, rhythm control is not necessary. The strategies of rate control and rhythm control result in similar clinical results with respect to symptoms, mortality, and stroke risk. Antiarrhythmic drug therapy and attempts at restoring sinus rhythm should thus be reserved for patients who are symptomatic and who do not tolerate the rhythm well. Since this patient is feeling well, his current treatment regimen is satisfactory and reassurance is the best option, as he should not be exposed to potential complications from antiarrhythmic drugs or invasive procedures.
Pulmonary vein ablation is an emerging therapy for atrial fibrillation. The procedure entails ablation around the left side of the heart, especially around the pulmonary veins. The best candidates are patients with paroxysmal atrial fibrillation. The success rate is approximately 70%, but the rate of complications is about 6%. The procedure should be reserved for patients with refractory atrial fibrillation and disabling symptoms.
Key Point
- Patients with atrial fibrillation and minimal symptoms can usually be managed with rate control alone (without rhythm control).